Most people think trauma is about “the past.”
But trauma is really about what your brain and body are still doing right now — especially when something in the present feels even the tiniest (sometimes completely imperceptible) bit like the danger you survived.
If you haven’t read “PTSD Breakdown – Part 1: You’re Not Crazy.” go do that first. Because we’re going deeper than the amygdala this time — The amygdala doesn’t just flip the “danger switch.” It disrupts the entire network responsible for thinking, planning, regulating your body and emotions, and just generally feeling safe in the world.
When triggers hit, you really do “lose your mind” — literally.
This post breaks down what actually happens inside the brain during trauma and why triggers can hijack your emotions, your body, your memory, and your ability to think clearly.
Revisiting the Prefrontal Cortex: The Brain’s CEO (and the First to Go Offline)
The prefrontal cortex (PFC) sits right behind your forehead. It’s the part of the brain responsible for:
- emotion regulation
- problem‑solving
- working memory
- planning and organization
- impulse control
- attention
- social behavior
- decision‑making
Basically: the PFC is the part of you that makes thoughtful, rational choices. When you’re calm, the PFC is in charge. When you’re triggered, the PFC experiences a hostile takeover.
Why?
Because the amygdala — the brain’s danger detector — doesn’t care about logic. Its job is survival, not accuracy. When the amygdala senses danger (whether you realize it in real-time or not), it sends a “shut it down” signal to the PFC. You’ve literally “lost your mind,” because the brain is doing its job — prioritizing survival over thinking.
This is why trauma survivors often say things like:
- “I knew it wasn’t a big deal, but I couldn’t stop reacting.”
- “I couldn’t think straight.”
- “I froze and couldn’t make a decision.”
- “I felt out of control.”
That’s not a personality flaw. It’s neurobiology. And it’s normal.
The Amygdala: It’s not just an alarm system.
We’ve learned about the amygdala as the fear center in my previous post. But it has a second job that explains almost every trauma trigger: The amygdala is also a sensory integration center.
It constantly scans:
- sights
- sounds
- smells
- textures
- facial expressions
- tone of voice
And it compares them to past danger.Your amygdala isn’t looking for meaning — it’s looking for matches.If anything resembles the original danger — even subconsciously — the amygdala fires the alarm, and the PFC is no longer in charge of what happens next. This is why trauma triggers often don’t make logical sense.
- A smell.
- A hallway.
- A season.
- A tone.
- A song.
- A look on someone’s face.
If there’s the slightest hint of a match, the amygdala goes to work.
Once the amygdala hits the alarm, it sends a message to the hypothalamus, which controls your physical stress response:
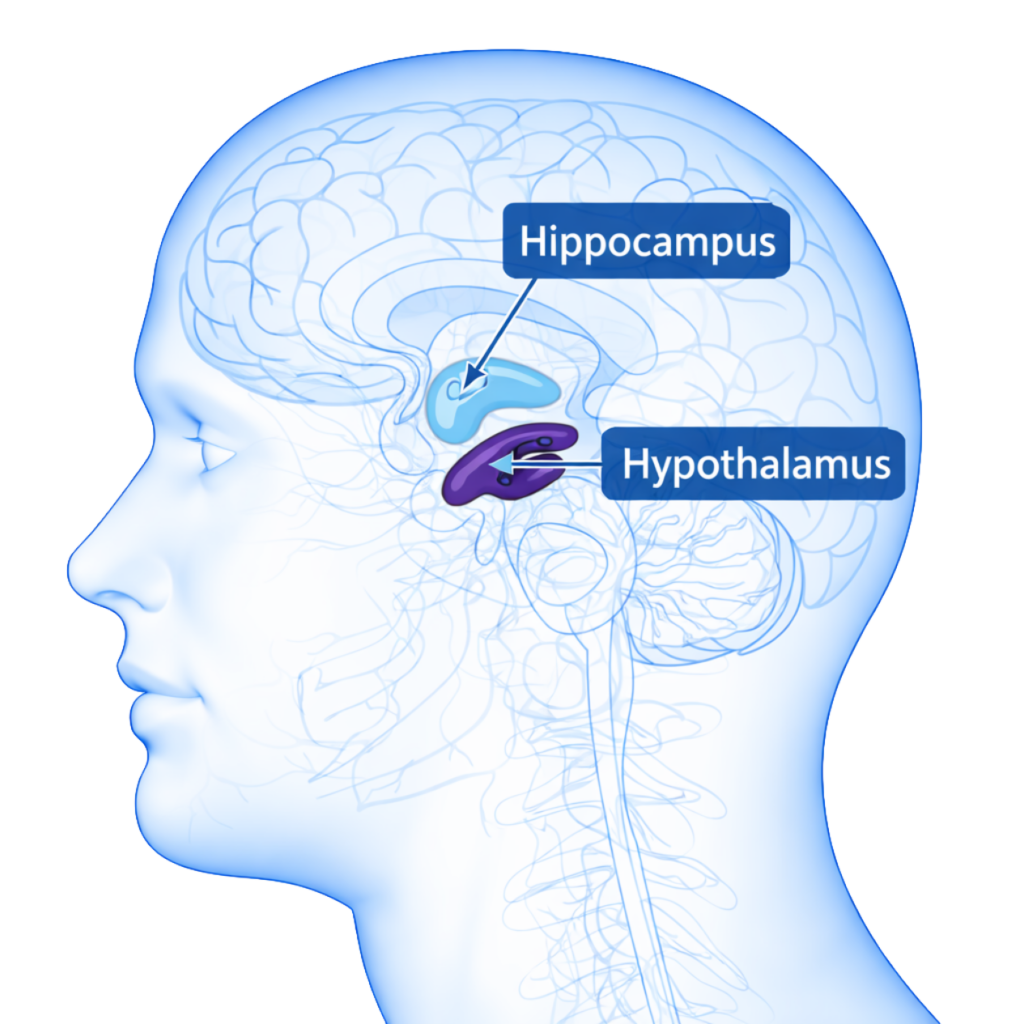
The Hypothalamus: The Body’s Stress Switch
- increased heart rate
- muscle tension
- shallow breathing
- stomach tightening
- sweating
- adrenaline & cortisol release
Your body reacts before you even know why. Trauma isn’t just “in your head.” It’s in your body.
The Hippocampus: The Memory + Emotion Coordinator
The hippocampus is the part of the brain that:
- forms new memories
- organizes memories
- links emotions to memories
- helps you tell past from present
Let’s go back to the American Psychological Association’s definition of trauma:
Trauma is a deeply distressing or disturbing experience that overwhelms an individual’s ability to cope.
During trauma, the amygdala is doing its job flooding the brain and body with everything it needs to survive. In doing so, the hippocampus can get overwhelmed. It can’t file the experience into long‑term memory properly, as it would regular everyday events. This leads to two major problems — and why PTSD makes you think you’re “crazy,” but you’re actually not, and here’s why:
Memories may be incomplete or fragmented
When the amygdala is firing, the prefrontal cortex is offline, and the hypothalamus is flooding the body with stress hormones, the hippocampus can’t fully do its job.
So memories become:
- fragmented
- blurry
- out of order
- missing
- stored as sensations instead of stories
- stored as emotions instead of words
People often say:
- “I can only remember pieces of what happened.”
- “I remember the smell.”
- “I remember the fear.”
- “I remember the ceiling.”
- “I remember being so cold.”
Emotions from the trauma get re‑attached to present triggers
When the hippocampus can’t file a memory away, the emotions just kinda float around, not knowing where to go. So when something in the present resembles the trauma, the amygdala activates, and the hippocampus pulls up the unprocessed emotional file and attaches it to the current moment.
This is why a small trigger can create a huge emotional reaction.
The Trigger Response Explained
Here’s the actual sequence:
Trigger → memory match (conscious or subconscious) → amygdala senses danger → prefrontal cortex goes offline → hypothalamus activates the stress response → hippocampus replays unprocessed emotions → cue trauma response (otherwise known as “overreacting.”)
This is why trauma reactions feel like ambushes that come out of nowhere. The reaction isn’t happening in the thinking part of the brain.
It’s happening in the survival system.
Conscious vs. Subconscious Trigger Examples
Conscious Example: Criticism → Perfectionism
Let’s say someone grew up in a home where mistakes were punished or shamed.
As an adult:
- A boss’s tone
- A partner’s feedback
- A teacher’s comment
- A coworker’s raised eyebrow
…can trigger the same fear response.
The amygdala hears criticism and thinks: “Danger. You’re about to be rejected, punished, or humiliated.” The PFC shuts down. The hippocampus pulls up the old emotional file. And suddenly perfectionism feels like the only way to stay safe.
Subconscious Example: Holiday Decorations → Irritability
This one confuses people.
Someone might say:
- “The holidays just stress me out.”
- “I hate the holidays and I don’t know why.”
- “Everyone else is happy — why do I just want to crawl in a hole?”
If the trauma happened in late fall, things like holiday décor, music, the smell of pine trees, cold weather, certain foods, or even visiting family members can trigger the danger response — even if the person has zero conscious awareness of the connection.
Remember, the amygdala doesn’t care about context or accuracy. It cares about sensory matches.Their prefrontal cortex is going offline.Their hypothalamus is firing the stress response (otherwise known as anxiety). And their hippocampus is pulling up old emotional files.
So for the person who “hates the holidays,” it’s not that the festivities are overwhelming. It’s that their brain and body are overwhelmed. There is too much going on — not in the room, but in the nervous system.
How Trauma Gets Stuck — and What the Brain Needs to Heal
When something overwhelming happens, the brain tries to process the emotional memory and file it away so it can become part of your past instead of something you keep reliving. A large part of this processing happens during a stage of sleep called REM sleep — the dream stage — when the brain sorts, organizes, and “files” emotional experiences. Think of REM as the brain’s overnight clean‑up crew.
But when trauma is too intense or too much to handle at once, that clean‑up process gets disrupted.
- REM sleep becomes lighter or more fragmented
- nightmares increase
- the brain keeps trying to process the trauma but can’t finish the job
- the emotional charge stays high
- the memory stays “unfiled” and easily triggered
This is why so many trauma survivors have nightmares, restless sleep, or wake up exhausted — the brain is trying to integrate the experience but keeps getting stuck in the middle of the job. And this is exactly why therapies like EMDR, that mimic REM processing are so effective — but that’s the next post.
Here’s the thing:
Trauma healing isn’t about “thinking differently.” You can’t out‑logic a survival system. You also can’t “positive mindset” your way out of a survival response. Healing requires:
- calming the amygdala so it stops firing false alarms
- re‑engaging the prefrontal cortex so you can think clearly again
- helping the hippocampus file the memory properly
- reducing the hypothalamus’s constant stress activation
- integrating the sensory, emotional, and memory networks so they work together
When these parts start working together again, triggers lose their power. The past stops hijacking the present.
Pulling It All Together — A Real Life Example
I once worked with a woman who had been sexually assaulted on her college campus. She remembered pieces of the event, but not all of it — which is normal when the hippocampus is overwhelmed. What she did remember was the fear, the freeze, and the feeling of being trapped.
Fast‑forward a year. She came to therapy because she having multiple panic attacks a day. She had to drop out of school and quit her job. She could barely leave the house. She was constantly on edge. She couldn’t function.
We decided to use EMDR to process what had happened to her. During one session, her brain finally connected the dots:
Her attacker was wearing a red shirt.
Okay — hold that.
Because here’s where the amygdala’s sensory‑matching job becomes painfully clear.
This woman worked at Target.
Every. Single. Employee.
Every. Single. Shift.
Red shirts. Everywhere.
The amygdala saw a red shirt → matched it to danger → fired the alarm → shut down her prefrontal cortex → activated her hypothalamus → pulled up the unprocessed emotional file from her hippocampus → and sent her into panic.
Her brain wasn’t broken. Her brain was doing exactly what brains do:
Protecting her.
The moment those dots came together, she cried — not because she was scared, but because she finally understood.
“I’m not crazy. My brain is trying to protect me.”
That’s the moment trauma survivors exhale for the first time.

