If you’re living with PTSD, you’ve probably had moments where you’ve thought:
- “Why am I like this?”
- “Why can’t I just get over it.”
- “Other people go through worse — what’s wrong with me?”
- “Why does my body freak out when nothing is happening.”
People with PTSD often assume they’re “broken,” dramatic, weak, or failing at being a functional human. But here’s the truth:
Your symptoms aren’t signs of damage — they’re signs that your brain is doing exactly what it was built to do.
PTSD isn’t a character flaw. It isn’t a lack of willpower. It isn’t a failure to “move on.”
It’s a normal biological response to an overwhelming experience. And once you understand what your brain is doing — and why — the whole picture starts to make a lot more sense.
Let’s break it down.
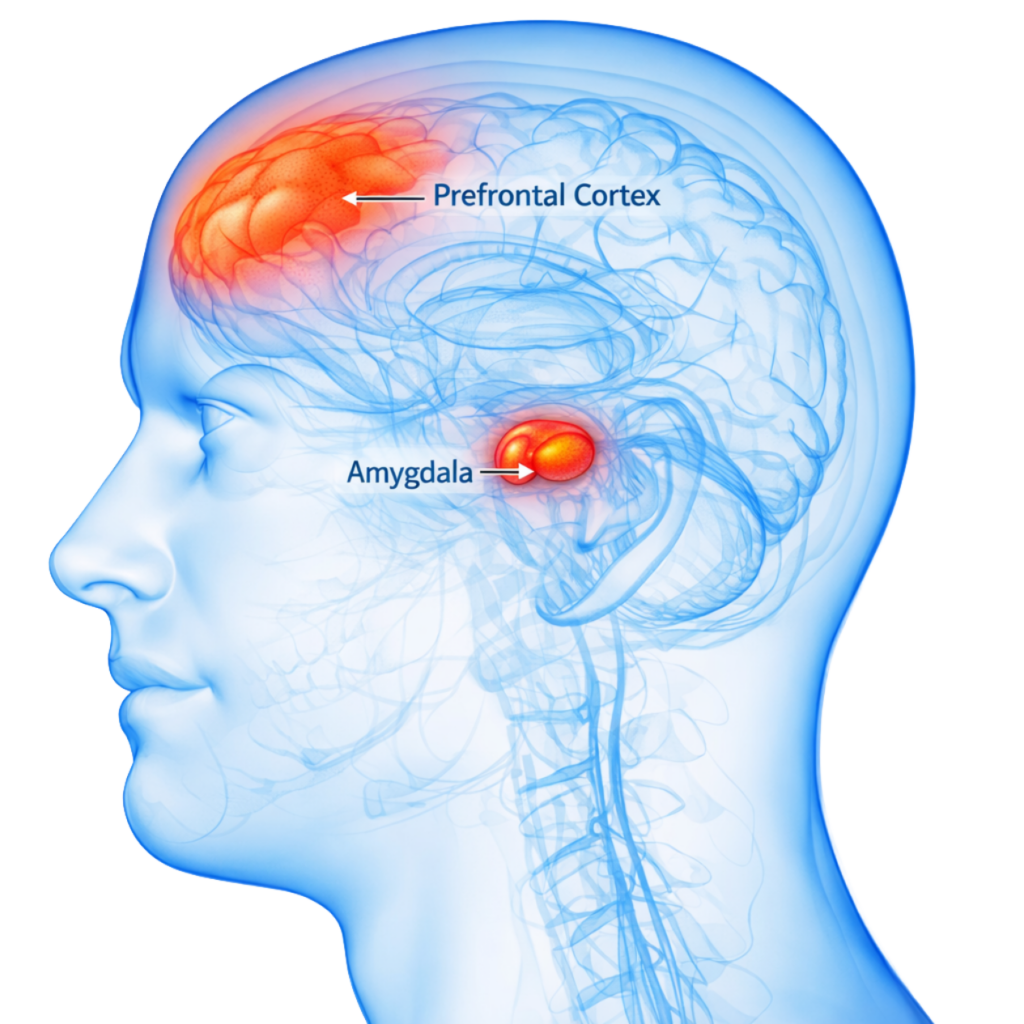
The Two Key Players:
The Amygdala & Prefrontal Cortex
There are many parts of the brain, but PTSD really comes down to two:
The Amygdala — Your Internal Alarm System
Think of the amygdala as the “boss of everything.” It’s the air‑traffic control tower of your brain, constantly scanning your environment for anything that even resembles danger. Its job is simple:
Keep you alive.
It does not care about nuance.
It does not care about context.
It does not care about your to‑do list, your relationships, or what’s for dinner.
It cares about survival. Period.
The Prefrontal Cortex — The Thinking Brain
This is the part of your brain responsible for:
- logic
- decision‑making
- planning
- emotional regulation
- executive functioning
It’s the part that helps you think, “Hmm, maybe I shouldn’t send that text,” or “I need to leave the house by 8:15.” But here’s the catch: The prefrontal cortex is slow.
The amygdala is fast. Lightening fast. And in a crisis, speed wins.
You + A Bear = No Time for Deep Thoughts
Imagine you’re taking a peaceful walk on a nature trail. Birds chirping. The sun is shining. All is well.
Then you see a bear.
You are not standing there weighing your options. You are not thinking about your grocery list. You are not wondering whether you left the stove on.You’re not thinking at all.
Why?
Because the instant your amygdala senses danger, your prefrontal cortex — the rational, logical, “let’s think this through” part of your brain — goes offline.
In about 20–50 milliseconds (roughly the speed of a lightning strike), your amygdala:
- floods your body with adrenaline
- increases your heart rate
- redirects blood flow to your muscles
- sharpens your senses
- prepares you to run, fight, or freeze
You don’t choose the response.Your brain chooses survival. This is not a glitch. This is not a malfunction.
This is your brain doing its job.
So What Does This Have to Do With PTSD?
Let’s start with the American Psychological Association’s definition of trauma:
Trauma is a deeply distressing or disturbing experience that overwhelms an individual’s ability to cope.
Trauma isn’t defined by the event — it’s defined by the nervous system’s response to the event. When the amygdala takes over, you might experience:
- tunnel vision
- racing heart
- shaking
- nausea
- sweating
- time slowing down or speeding up
- difficulty speaking
- difficulty thinking clearly
- feeling “checked out” or disconnected
This is not you “freaking out” for no good reason. This is your nervous system shifting into survival mode.
Facing down a bear? Traumatic.
A violent event? Traumatic.
A medical emergency? Traumatic.
Growing up in a home where you never felt safe? Traumatic.
Being chronically criticized, ignored, or shamed? Traumatic.
After a traumatic experience, the amygdala stays on high alert. The prefrontal cortex — the part that helps you make sense of what happened — hasn’t fully processed the event yet. Your nervous system doesn’t realize — the bear is gone now.
How Trauma Memories Get Stored (And Why They Feel “Unfinished”)
Traumatic memories don’t get stored like normal memories. Normal memories get filed away neatly in the brain’s “story” section — with a beginning, middle, and end. Trauma memories get stored in the sensory part of the brain:
- images
- sounds
- smells
- body sensations
- emotions
They’re fragmented, disorganized, and lack a timestamp. They don’t feel like “something that happened.” They feel like “something that is happening right now.” the prefrontal cortex hasn’t finished processing the memory, the amygdala treats it as unfinished business.
This is why people with PTSD often say:
- “It feels like I’m back there.”
- “My body reacts before I even know what’s happening.”
- “I know I’m safe, but it doesn’t feel like it.”
Six Months Later… Why a Teddy Bear Can Trigger Panic
Let’s go back to our bear example.
Six months after the attack, you’re at a child’s birthday party. Someone unwraps a teddy bear. It’s soft, cute, and harmless. Right?
But your amygdala doesn’t see “cute.” It sees a bear‑shaped object and immediately pulls the fire alarm. With lightening speed, your body reacts as if the original threat is happening again:
- adrenaline surge
- racing heart
- panic
- urge to run or hide
You don’t think your way into this reaction — and you can’t think your way out of it. The prefrontal cortex is offline again.If it were online, you’d say, “Oh, it’s just a stuffed animal,” and move on. But when trauma is unprocessed, the amygdala treats anything even vaguely similar to the original danger as a threat.
Other Everyday Triggers People Don’t Realize Are Trauma‑Related
A trigger can be anything that resembles — even very loosely — the original danger:
- a slammed door
- a certain cologne
- a hospital hallway
- a tone of voice
- a song
- a date on the calendar
- a facial expression
- a particular weather pattern
- a phrase someone says
- a certain type of lighting
Your amygdala is not trying to ruin your life. It’s trying to keep you alive. It would rather be wrong 1,000 times than miss danger once.
What “Fight” and “Freeze” Responses Can Look Like in Real Life
Most people understand “flight” — the urge to get the hell out of there. Because — a bear. But day-to-day fight and freeze responses are often unrecognized.
A trauma‑driven fight response can look like:
- snapping at someone over something small
- feeling instantly irritated or overwhelmed
- needing to defend yourself even when you’re not being attacked
- feeling a surge of anger or intensity you can’t explain
- talking fast, pacing, or feeling “amped up”
This isn’t you being “dramatic” or “overreacting.” It’s your nervous system trying to create enough intensity to scare off a threat — even when there is no bear.
Freeze is the most misunderstood survival response. It doesn’t mean “calm.” A freeze response can look like:
- going numb
- feeling stuck or paralyzed
- shutting down emotionally
- going quiet mid‑conversation
- feeling like you’re watching yourself from the outside
- losing the ability to speak or move
- feeling disconnected from your body
Just like flight or fight, a freeze response is not a choice. It’s not passivity. It’s not weakness. It’s your brain slamming the brakes because it believes escape is impossible.
Fight, flight, and freeze responses are automatic survival strategies, not personality traits.
“Why Can’t I Just Get Over It.”
This is one of the most painful questions people with PTSD ask themselves. The answer is actually quite simple:
Because you can’t logic your way out of a survival response.
The prefrontal cortex — the logical part — is offline during a trigger. The amygdala — the survival part — is in charge.
You can’t out‑think adrenaline.
You can’t out‑reason a nervous system that is still trying to outrun a bear.
“Just calm down” is not an option.
It’s easy to confuse “getting over it” with avoidance. We want to tuck it away and not think about it anymore. However, avoidance actually strengthens the alarm system. Every time you avoid a trigger, the amygdala learns: “Good job. Avoiding kept us alive. Let’s keep doing that.”
This is not a personal failure. This is neuroscience.
The Good News: Your Brain Is Normal
PTSD symptoms can affect every part of your life — relationships, work, school, parenting, sleep, and your sense of safety in the world. But the presence of these symptoms doesn’t mean you’re broken. In fact, quite the opposite is true. It means:
- your amygdala is doing its job
- your brain is trying to protect you
- the traumatic memory hasn’t been fully processed
- your prefrontal cortex can’t come online when you need it
You’re not “crazy.” You’re not weak. You’re not failing.
You’re having a normal biological response to an abnormal experience.
Your brain isn’t broken. It’s trying to protect you. It just needs a little help turning the alarm system off.
And here’s the cool part: The brain can rewire.
Neuro-based therapies — including EMDR, biofeedback, and somatic (body-based) therapies — help the brain reconnect the amygdala and the prefrontal cortex so the memory can finally be filed away as “over.”
The bear goes away. You can breathe again.

